|
9/2/2023 0 Comments Single fixed dilated pupilIn an unconscious patient, the best response is localization, in which she reaches across the midline toward the stimulus site as though trying to stop the pain. (See Testing your patient’s response to pain.) Then watch for specific motor responses, as specified in the GCS. 
To assess motor response using the GCS, apply a painful or other noxious stimulus to a central part of the body for instance, use trapezius squeezing, supraorbital pressure, earlobe pinching, or a sternal rub. An unconscious patient is likely to open her eyes only in response to pain, if at all obviously, you can’t test her best verbal response at all. To determine if the patient is unconscious and unable to follow commands, use the Glasgow Coma Scale (GCS) to test eye opening, best motor response, and best verbal response. Once you’ve established that your patient is stable enough to assess, begin the neuro exam itself. Assess LOC, eye opening, and motor response Be aware that a temporary decline in neurologic status caused by insufficient oxygenation or circulation still represents a neurologic change-and leads to permanent neurologic loss unless the underlying problem is corrected. Ideally, you should conduct the neuro exam when the patient’s blood pressure, temperature, heart rate, and heart rhythm are normal. To appropriately assess the patient’s peak neurologic status, be sure to evaluate oxygenation and circulation. Next, check vital signs: Are her respirations adequate? Are her vital signs stable? Is her blood pressure high enough to perfuse the brain and other vital organs? Be aware that current or progressive injury to the brain and brain stem may make vital signs unstable, but this situation can be complex: Although unstable vital signs can reduce neurologic response, brain injury itself may cause unstable vital signs. Ask yourself: Is the airway patent? If so, is the patient able to maintain it? First step: Evaluate ABCs and vital signsĪs with any patient, give top priority to assessing the ABCs-airway, breathing, and circulation. Yet despite the relative brevity of this type of exam, it can yield a significant amount of information. If your patient can’t follow commands, you’ll be able to assess only the pupils, eye opening, motor response, and some of the cranial nerves. If she can, your exam can be more comprehensive and should include evaluation of: The type of neuro exam you conduct depends on whether your patient can follow commands. Once you’ve completed the initial assessment, subsequent assessments can be either basic or more in-depth. Performing it early is crucial because this helps you establish a baseline for later comparison.įor accurate interpretation of assessment findings, nurses on the offgoing and oncoming shifts should evaluate the patient’s neurologic status together during shift changes or care transfers (as well as with the medical team on rounds). It starts the moment you meet the patient.  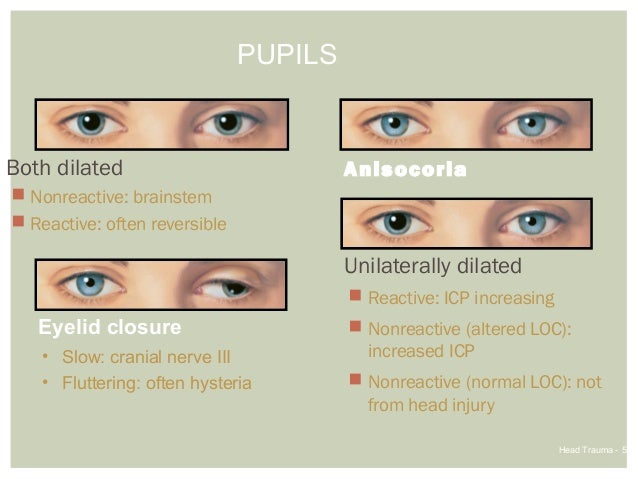
The neuro exam can be conducted quickly and is easy to integrate into your daily assessment. One reason may be that, unlike CT scans and other diagnostic tools, its results come in shades of gray, not black and white. Although it’s still an integral assessment component for critically ill patients, many bedside nurses overlook or underuse it. Subtle changes in findings may indicate the need for further testing.īefore the advent of computed tomography (CT) in the 1970s, the neurologic examination was the main tool used to monitor a patient’s neurologic condition. But once you become proficient in performing this exam, you’ll be able to detect early significant changes in a patient’s condition-in some cases, even before these show up on more advanced diagnostic tests.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
